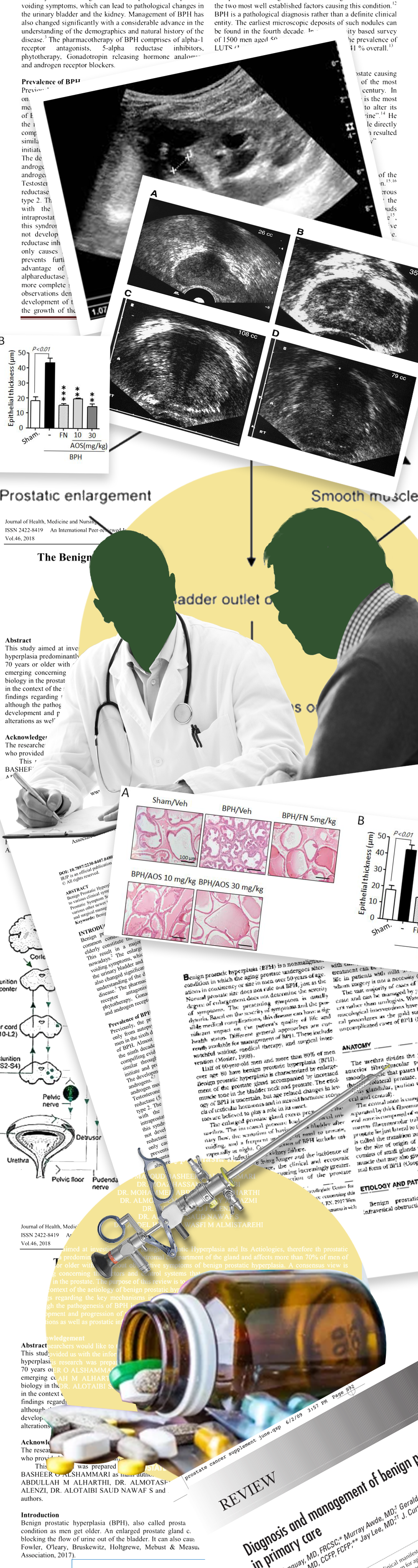
Benign Prostate Hypertrophy, also known as Benign Prostatic Hyperplasia, is a noncancerous enlargement of the prostate gland — a common condition as men age. The prostate surrounds the urethra, and its enlargement can block urine flow.
BPH is not prostate cancer and doesn’t increase the risk of it. However, it can cause uncomfortable urinary symptoms and affect quality of life.
BPH is addressed when it causes bothersome urinary symptoms such as:
Frequent or urgent need to urinate
Increased urination at night (nocturia)
Difficulty starting urination
Weak urine stream or stream that stops and starts
Dribbling at the end of urination
Inability to completely empty the bladder
Complications that may arise and justify treatment:
Urinary tract infections (UTIs)
Bladder stones
Bladder or kidney damage
Acute urinary retention (sudden inability to urinate)
Initial evaluation includes:
Digital rectal exam (DRE) to assess prostate size
Urine test to rule out infection
Prostate-specific antigen (PSA) blood test to screen for cancer
Uroflowmetry to measure urine flow rate
Postvoid residual volume test via ultrasound
No surgical access is needed unless procedural treatment is chosen.
Treatment depends on severity:
For mild symptoms: limit fluids at night, avoid caffeine/alcohol, double voiding.
Alpha blockers (e.g., tamsulosin): relax prostate muscles to ease urine flow.
5-alpha reductase inhibitors (e.g., finasteride): shrink the prostate over time.
Combination therapy: uses both for better results.
Tadalafil: also FDA-approved for BPH.
Transurethral Microwave Therapy (TUMT)
Transurethral Needle Ablation (TUNA)
TURP (Transurethral Resection of the Prostate): gold standard.
Laser therapy (e.g., HoLEP)
Prostatectomy for very large prostates
Prostatic urethral lift (UroLift) or Rezūm water vapor therapy
Many men notice symptom relief with medication in a few weeks.
Minimally invasive therapies and surgeries can offer long-term relief.
Recovery after surgery may include short-term catheter use.
Sexual side effects (e.g., retrograde ejaculation) can occur, depending on treatment.
Medication side effects: dizziness, ejaculatory dysfunction, reduced libido.
Surgical risks: bleeding, infection, incontinence, sexual dysfunction.
Bladder damage if left untreated.
Urinary retention may require emergency catheterization.
Medications are effective in reducing symptoms by 30–50% in most men.
Surgical options like TURP have high success rates and long-term relief.
Quality of life often improves significantly after effective treatment.
Avoid drinking large volumes of fluid at once, especially before bed.
Limit caffeine and alcohol.
Regular follow-ups for PSA and symptom monitoring.
Pelvic floor exercises may help with urinary control post-surgery.
Urologist: primary specialist for diagnosis and treatment
Primary care provider: monitors PSA, manages medications
Nursing staff: catheter care, post-op instructions
Clinical trials are evaluating:
New drug combinations
Minimally invasive approaches
Prostatic artery embolization