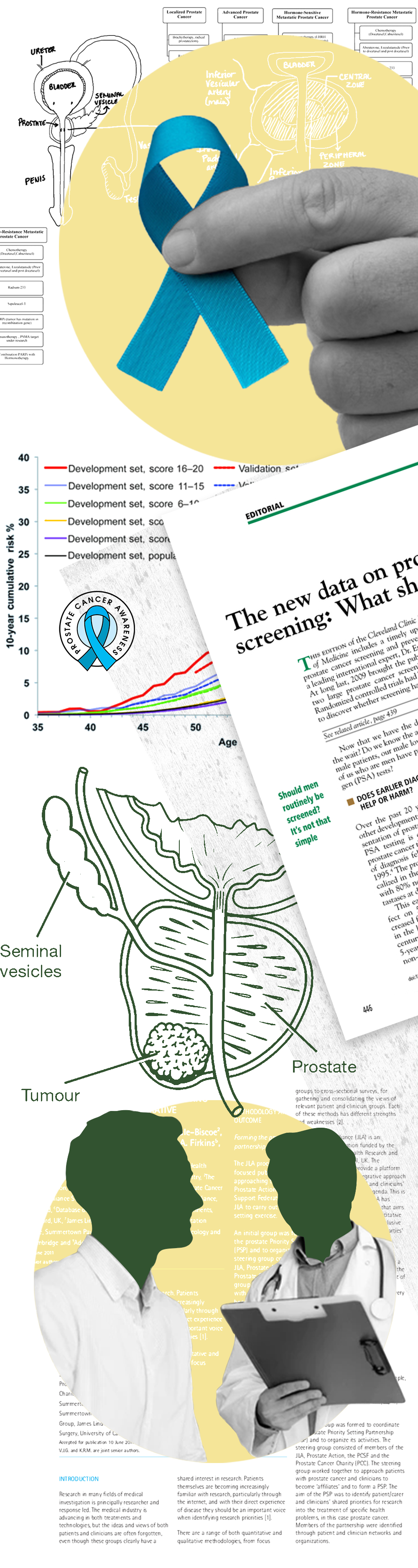
Prostate cancer is a malignancy in the prostate gland, a small, walnut-sized organ in men located just below the bladder and in front of the rectum. It produces seminal fluid that nourishes and transports sperm.
Prostate cancer is one of the most common cancers in men and typically grows slowly. Some types remain confined to the prostate and may not cause serious harm, while others can be more aggressive and spread quickly.
Screening and evaluation are done:
Due to age-related risk: Most cases appear in men over 50.
To detect early-stage cancer, often before symptoms arise.
If symptoms like urinary problems, blood in urine/semen, erectile dysfunction, or bone pain occur.
When PSA levels are elevated or abnormalities on digital rectal exam (DRE) are found.
If there’s a family history or genetic predisposition (e.g., BRCA mutations)i
Before diagnosis or treatment:
Blood tests: Prostate-specific antigen (PSA)
Digital Rectal Exam (DRE)
Biopsy: Usually transrectal ultrasound-guided
MRI or CT scans to assess tumor extent
Bone scan if metastasis is suspected
For treatment access:
Consultations with urologists, oncologists, radiologists
Referral to cancer treatment centers
Genetic counseling if family history is present
Diagnosis:
PSA test → DRE → Prostate biopsy
Gleason score assigned to assess aggressiveness
Treatment options:
Active Surveillance (for low-risk, localized cancer)
Surgery – Radical prostatectomy (open or robotic-assisted)
Radiation Therapy – External beam or brachytherapy
Hormone (Androgen Deprivation) Therapy – Reduces testosterone
Chemotherapy – For advanced or hormone-resistant cases
Immunotherapy / Targeted therapy – In metastatic or genetic variants
Many men with early-stage prostate cancer live normal life spans without immediate treatment.
Post-surgical effects: urinary incontinence, erectile dysfunction
Side effects of radiation: fatigue, bowel/urinary changes
Hormone therapy may cause hot flashes, loss of libido, bone thinning
Long-term monitoring of PSA levels is essential
Advanced stages require systemic treatment and palliative care
Urinary incontinence or dribbling
Erectile dysfunction
Infertility (surgical or radiation-induced)
Bowel issues with radiation
Bone loss and muscle weakness from hormone therapy
Psychological impact: anxiety, depression, body image issues
Rarely:
Blood clots post-surgery
Lymphedema
Secondary cancers due to radiation
Five-year survival rate for localized prostate cancer: ~98–100%
Early detection = best outcome
PSA levels used to monitor recurrence
Aggressive or metastatic cancers require ongoing management
Advances in personalized therapy are improving prognosis
Regular PSA checks and physical exams
Lifestyle guidance:
Low-fat, plant-rich diet
Exercise
Stress management
Pelvic floor exercises after surgery
Monitor for bone health if on hormone therapy
Emotional support, especially during active surveillance
Care Team Includes:
Urologist: Surgical treatment, follow-ups
Oncologist: Chemotherapy, hormone therapy
Radiation Oncologist: Planning and delivering radiation
Nurse Navigator: Coordinates care
Psychologist/Social Worker: Mental health support
Physiotherapist: Pelvic floor rehab
Clinical Trials:
Immunotherapy advancements (e.g., checkpoint inhibitors)
Genetic testing and targeted therapy (e.g., PARP inhibitors)
Novel hormonal agents
Vaccine trials (like Sipuleucel-T