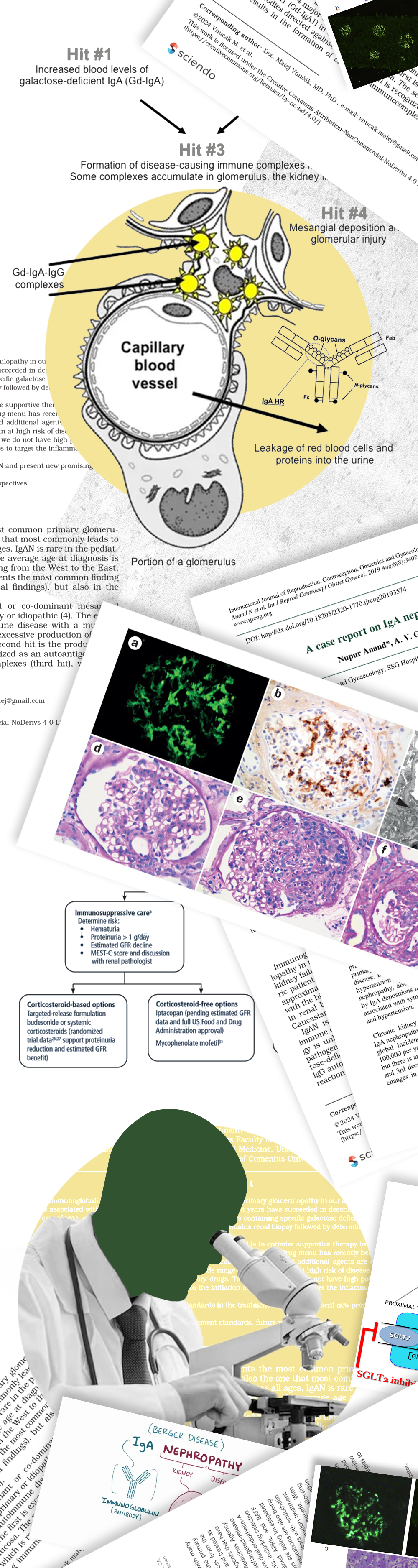
IgA Nephropathy, also called Berger’s disease, is a kidney disorder that occurs when an antibody called immunoglobulin A (IgA) builds up in the kidneys. This buildup causes inflammation that can damage the glomeruli (tiny filters of the kidneys). Over time, the condition may lead to blood in the urine, protein leakage, high blood pressure, and progressive kidney damage.
Evaluation for IgA Nephropathy may be needed if:
You notice blood in urine (visible or microscopic).
Urine is foamy/frothy (a sign of protein loss).
You have high blood pressure or swelling in legs and ankles.
Blood tests show reduced kidney function.
You have recurrent infections or immune-related illnesses that trigger kidney problems.
Diagnostic steps usually include:
Urine tests: To check for blood and protein.
Blood tests: To measure kidney function (creatinine, eGFR).
Kidney biopsy: The gold standard to confirm IgA deposits in kidney tissue.
Imaging: Ultrasound may help evaluate kidney structure, but is not diagnostic.
Preparation is minimal for blood/urine tests. For biopsy, hospital admission, fasting, and monitoring may be required.
Urine & blood analysis: Initial screening for abnormalities.
Kidney biopsy: A small tissue sample is taken with a needle and examined under a microscope to detect IgA deposits.
Treatment:
Blood pressure medications (ACE inhibitors, ARBs).
Corticosteroids or immunosuppressants in certain cases.
Fish oil or newer therapies (like targeted immunomodulators) in select patients.
Early disease may not cause noticeable symptoms.
Some patients experience recurrent episodes of blood in urine after infections.
For many, the disease progresses slowly, over years.
A percentage of patients may develop chronic kidney disease (CKD) or kidney failure if untreated.
Regular follow-ups are needed to monitor kidney function and control blood pressure.
If unmanaged, IgA Nephropathy can cause:
High blood pressure.
Chronic kidney disease.
End-stage renal failure.
Nephrotic syndrome (severe protein loss in urine).
Increased cardiovascular risk due to hypertension and CKD.
The disease course is highly variable: some patients live a normal lifespan with little progression, while others experience significant kidney decline.
Treatments help control symptoms and slow progression but currently there’s no definitive cure.
Clinical outcomes depend on blood pressure control, level of protein in urine, and overall kidney health at diagnosis.
Low-salt diet to manage blood pressure.
Regular exercise and weight management.
Avoid smoking and limit alcohol.
Take prescribed medications consistently.
Monitor blood pressure and kidney function as advised.
Nephrologist: Leads diagnosis, treatment, and follow-up.
Pathologist: Confirms biopsy findings of IgA deposits.
Dietitian: Guides nutrition to support kidney health.
Nursing team: Supports medication compliance and patient education.
Clinical trials: Ongoing studies are exploring targeted immunotherapies and biologics that may alter disease progression in the future.