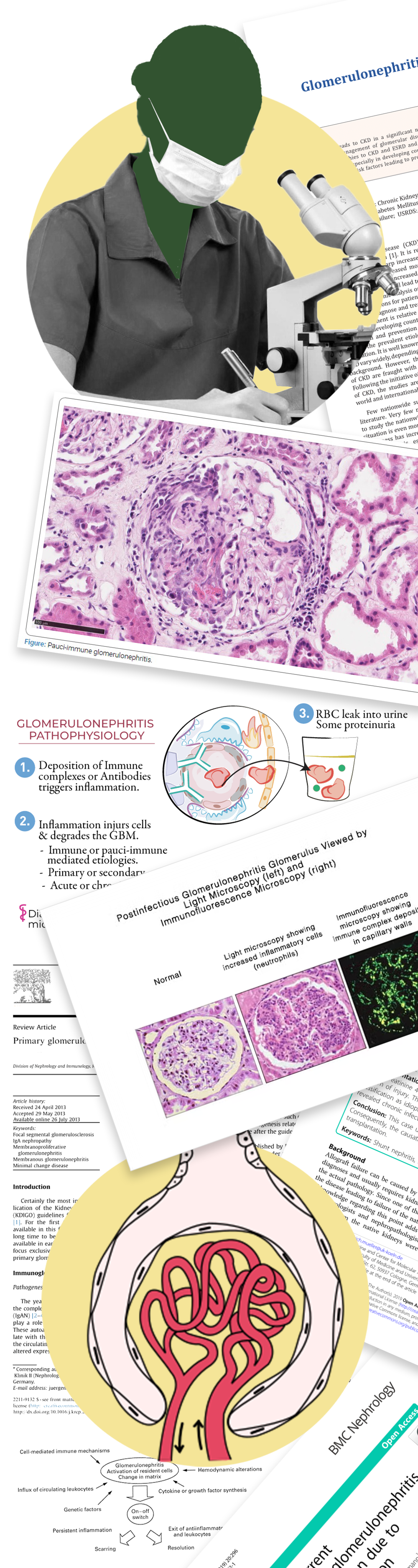
Glomerulonephritis, also called GN, is an inflammation of the glomeruli, which are small structures present in the kidneys and made up of tiny blood vessels (capillaries). You have almost a million of them. These knots of vessels help filter blood, remove excess fluids, electrolytes, and waste products from the bloodstream and proceed them into the urine. If the glomeruli become inflamed and scarred, kidneys will stop working properly, ultimately resulting in kidney failure.
GN can be both acute, sudden, chronic, or long-term. This condition used to be known as Bright’s disease.
There are two main types of glomerulonephritis.
A sudden onset of kidney inflammation often caused by infection but can also occur due to autoimmune disorders etc. It can get better by treating the cause so the right treatment should be started as soon as possible.
When it develops silently (without symptoms) over several years. It can lead to kidney failure. Treatment can help keep the disease from getting worse. Nearly all forms of acute glomerulonephritis can progress to chronic glomerulonephritis depending on the underlying cause. Important causes include primary glomerular diseases (like FSGS, MPGN, Membranous nephropathy, etc), autoimmune conditions (like lupus nephritis, ANCA-related vasculitis, etc.), certain infections and medications.
Rapidly progressive glomerulonephritis
Loss of kidney function over a very short period (days to weeks).
It is important to note that some people can have an acute attack of glomerulonephritis and then develop chronic glomerulonephritis years later.
The various signs and symptoms linked with Glomerulonephritis have been divided into the following three stages.
Puffiness in the facial area
Decrease in urine output
Blood in your urine, which turns your urine a dark rust color
Extra fluid in the lungs causes coughing
High blood pressure levels
The chronic form of nephritis can crop up without any significant symptoms. Some of the peculiar symptoms comprise:
Blood or excess protein in your urine, which may be microscopic and show up in urine tests
High blood pressure
Fluid retention (edema) with swelling evident in your face and ankles
Frequent nighttime urination
Bubbly or foamy urine, from excess protein
Abdominal pain
Frequent nosebleeds
While most patients with acute glomerulonephritis may present with symptoms as described above, many patients with chronic glomerulonephritis may be relatively free of any symptoms, even when kidney function has declined significantly. Some of the symptoms of this include:
Lack of appetite
Nausea or vomiting
Fatigue, insomnia
Dry, itchy skin
Shortness of breath
muscle cramps at night
There are many that cause glomerulonephritis. Sometimes, the disease runs in families and has a genetic factor involved, whereas in other cases, the cause of glomerulonephritis is completely unknown. Conditions that can lead to glomerulonephritis include:
Post-streptococcal Glomerulonephritis: Glomerulonephritis may develop in a patient around two to three weeks post-recovery from a throat infection or, rarely, a skin infection called impetigo. To fight against the infection, the body produces antibodies that accumulate in the glomeruli, causing inflammation. Children are more prone to develop post-streptococcal glomerulonephritis than adults, and they're also more likely to recover quickly.
Bacterial Endocarditis: Occasionally, the bacteria can spread through the bloodstream and accumulate in the heart, causing an infection of one or more heart valves.
Patients with a heart defect, such as a damaged or artificial heart valve, are at a greater risk of developing this condition.
Viral infections: Certain viral infections, HIV, hepatitis B, and hepatitis C, can end up provoking glomerulonephritis.
Lupus: Being a chronic inflammatory disease, this can influence several parts of the body, including skin, joints, kidneys, blood cells, heart, and lungs.
Goodpasture's syndrome: A rare immunological disorder due to an abnormal antibody, which can partially damage kidneys and lungs.
IgA nephropathy: This primary glomerular disease results from the deposition of immunoglobulin A (IgA) in the glomeruli. It is the most common primary glomerular disease.
Others include FSGS, MPGN, membraneous nephropathy, etc.
Vasculitis is inflammation of blood vessels. Types of vasculitis that can cause glomerulonephritis include:
Polyarteritis: This form of vasculitis affects medium and small blood vessels in many parts of your body, including the kidneys, skin, muscles, joints and digestive tract.
Granulomatosis with polyangiitis: This form of vasculitis, formerly known as Wegener's granulomatosis, affects small and medium blood vessels in your lungs, upper airways and kidneys.
Sclerotic conditions: Some diseases or conditions cause scarring of the glomeruli that results in poor and declining kidney function. These include:
High blood pressure: Long-term, poorly managed high blood pressure can cause scarring and inflammation of the glomeruli. Glomerulonephritis inhibits the kidney's role in regulating blood pressure.
Diabetic kidney disease (diabetic nephropathy): High blood sugar levels contribute to scarring of the glomeruli and increase the rate of blood flow through the nephrons.
Focal segmental glomerulosclerosis: In this condition, scarring is scattered among some of the glomeruli. This may be the result of another disease, or it may occur for no known reason.
In addition to the mentioned cases above, glomerulonephritis is associated with certain types of cancers, such as multiple myeloma, lung cancer, and chronic lymphocytic leukaemia (CLL).
In some cases, glomerulonephritis can be caused by certain drugs. For example, analgesic nephropathy is caused by heavy and prolonged use of certain pain relievers (analgesics), including the nonsteroidal anti-inflammatory drugs (NSAIDs), like ibuprofen and naproxen.
Sometimes, chronic glomerulonephritis is caused by Alport syndrome, an inherited genetic disease that damages the kidneys.
There are a number of risk factors that can increase the chances of developing glomerulonephritis, including:
Having a family history of kidney disease
Having an autoimmune condition, such as lupus or rheumatoid arthritis
Viral (strep throat or hepatitis B) or bacterial infections such as bacterial endocarditis
Taking certain medications, such as antibiotics or blood pressure medications
Being exposed to certain toxins, such as lead or mercury
The first step in diagnosis is a urinalysis test. Blood and protein in urine are important markers for the disease. A routine physical exam for another condition can also lead to the discovery of GN.
More urine testing may be necessary to check for important signs of kidney health, including:
Creatinine clearance
Total protein in the urine
Urine concentration
Urine specific gravity
Urine red blood cells
Urine osmolality
Blood tests may show:
Anemia, which is a low level of red blood cells
Abnormal albumin levels
Abnormal blood urea nitrogen
High creatinine levels
Your doctor may also order immunology testing to check for:
Antiglomerular basement membrane antibodies
Antineutrophil cytoplasmic antibodies
Antinuclear antibodies
Complement levels
Results of this testing may show your immune system is damaging your kidneys.
A biopsy of your kidneys may be necessary to confirm the diagnosis. This involves analyzing a small sample of kidney tissue taken by a needle.
To learn more about your condition, you may also have imaging tests such as the following:
CT scan
Kidney ultrasound
Chest X-ray
Intravenous pyelogram
Treatment options depend on the type of GN you’re experiencing and its cause.
One treatment is to control high blood pressure, especially if that’s the underlying cause of the GN. Blood pressure may be very hard to control when your kidneys aren’t working properly. If this is the case, your doctor may prescribe blood pressure medications, including angiotensin-converting enzyme inhibitors, or ACE inhibitors, such as:
Captopril
Lisinopril (Zestril)
Perindopril (Aceon)
Your doctor may also prescribe angiotensin receptor blockers, or ARBs, such as:
Losartan (Cozaar)
Irbesartan (Avapro)
Valsartan (Diovan)
Corticosteroids may also be used if your immune system is attacking your kidneys. They reduce the immune response.
Another method to reduce immune-triggered inflammation is plasmapheresis. This process removes the fluid part of your blood, called plasma, and replaces it with intravenous fluids or donated plasma that contains no antibodies.
For chronic GN, you’ll need to reduce the amount of protein, salt, and potassium in your diet. Additionally, you must watch how much liquid you drink. Calcium supplements may be recommended, and you may need to take diuretics to reduce swelling. Check with your general practitioner or kidney specialist for guidelines about diet restrictions or supplements. They can set you up with a medical dietician to advise you on your choices.
If your condition becomes advanced and you develop kidney failure, you may need to have dialysis. In this procedure, a machine filters your blood. Eventually, you may need a kidney transplant.
People with glomerulonephritis may need to follow a healthy diet that is low in salt and cholesterol. Reducing sodium (salt) in your diet can help lower blood pressure and control swelling (edema). Lowering cholesterol in your diet can help reduce the risk for heart disease. You might also need to lower your fluid and water intake. It is important to work with a registered dietitian to discuss any changes needed in your diet.
The following complications can also occur due to glomerulonephritis:
Acute kidney injury
Chronic kidney disease
Electrolyte imbalance, such as high levels of sodium or potassium
Congestive heart failure due to retained fluid or fluid overload
Pulmonary oedema due to retained fluid or fluid overload
High blood pressure
Malignant hypertension, which is rapidly increasing high blood pressure
Increased risk of infections
Blood clots, including deep vein thrombosis (DVT) or pulmonary embolism (PE).
High cholesterol.
Kidney failure, which can happen quickly or after several years.
Nephrotic syndrome (nephrosis), with protein in your pee, often leading to foamy pee and swelling in your body.
Chronic urinary tract infections
If caught early, acute Glomerulonephritis can be temporary and reversible. Chronic Glomerulonephritis may be slowed with early treatment. If Glomerulonephritis worsens, it can lead to reduced kidney function, chronic kidney failure, and end-stage renal disease.
Management of glomerulonephritis typically involves treating the underlying cause, managing symptoms, and controlling blood pressure and proteinuria. This may include medications, dietary changes, and lifestyle modifications.
The treatment for glomerulonephritis depends on the specific type and cause of the condition. It may involve medications, such as corticosteroids or immunosuppressants, lifestyle changes, and managing underlying health issues.
The curability of glomerulonephritis depends on the underlying cause and type. Some forms may be curable when the underlying condition is treated, while others may be managed but not entirely cured.