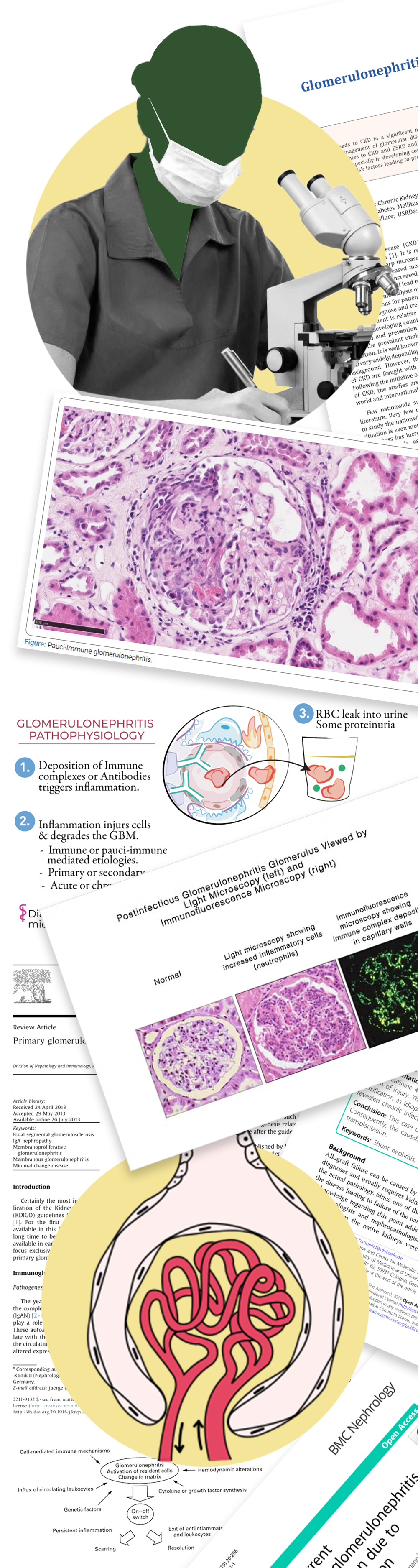
Glomerulonephritis (GN) refers to a group of kidney disorders where the glomeruli—the tiny filters in the kidneys—become inflamed or damaged. This inflammation reduces the kidney’s ability to remove waste and excess fluid from the blood.
The Glomerulonephritis Clinic at KKI provides specialized evaluation, diagnosis, and treatment for patients with both acute and chronic forms of GN, as well as GN linked with systemic diseases such as lupus or vasculitis.
Patients are referred to the GN Clinic if they have:
Blood in urine (hematuria) or foamy urine from protein leakage.
Swelling in the face, legs, or abdomen.
High blood pressure that’s difficult to control.
Declining kidney function detected on blood tests.
Family history of kidney disease or autoimmune conditions.
The clinic ensures early detection and targeted management to prevent kidney failure.
Before or during your clinic visit, you may need:
Urine tests: Protein, blood, or 24-hour urine collection.
Blood tests: Kidney function, autoimmune markers, cholesterol.
Imaging: Ultrasound to check kidney size and structure.
Kidney biopsy: Sometimes required to determine the exact type of GN.
Patients should bring prior medical records, medications, and lab reports to streamline care.
During the clinic visit:
A nephrologist will review your medical history and symptoms.
Diagnostic tests are ordered and interpreted.
Based on findings, treatment may include:
Immunosuppressants (e.g., corticosteroids, cyclophosphamide, biologics).
Supportive therapy (blood pressure control, ACE inhibitors/ARBs, diuretics).
Dialysis planning in advanced cases.
Patients with systemic diseases like lupus are managed in coordination with other specialists.
Initial visit: Comprehensive evaluation, baseline tests, and treatment initiation.
Follow-ups: Regular monitoring every few weeks/months depending on disease activity.
Long-term care: Ongoing adjustments to medications, infection prevention, and relapse management.
Most patients require continuous care, as GN can relapse or progress.
If untreated or poorly controlled, GN may cause:
Chronic kidney disease (CKD) and kidney failure.
Nephrotic syndrome (high protein loss, swelling, infections).
Severe hypertension and cardiovascular risk.
Increased risk of blood clots and infections (from disease and immunosuppressive drugs).
Early diagnosis and treatment can prevent irreversible kidney damage.
Many forms of GN respond well to immunosuppressive therapy.
Outcomes depend on GN subtype (Minimal Change, FSGS, Membranous, IgA, Lupus nephritis).
With proper follow-up, progression to dialysis or transplant can be delayed or prevented.
Patients are advised to:
Follow a low-salt, kidney-protective diet.
Take medications regularly as prescribed.
Monitor blood pressure at home.
Avoid smoking, excess alcohol, and unnecessary over-the-counter drugs (esp. NSAIDs).
Stay updated on vaccinations (to lower infection risk on immunosuppressants).
Nephrologist: Primary care for GN diagnosis and treatment.
Pathologist: Interprets kidney biopsy results.
Dietitian: Provides renal nutrition guidance.
Nurses: Monitor medications, follow-up compliance, and patient education.
Clinical trials: KKI participates in research on novel biologics, targeted therapies, and precision medicine for GN.