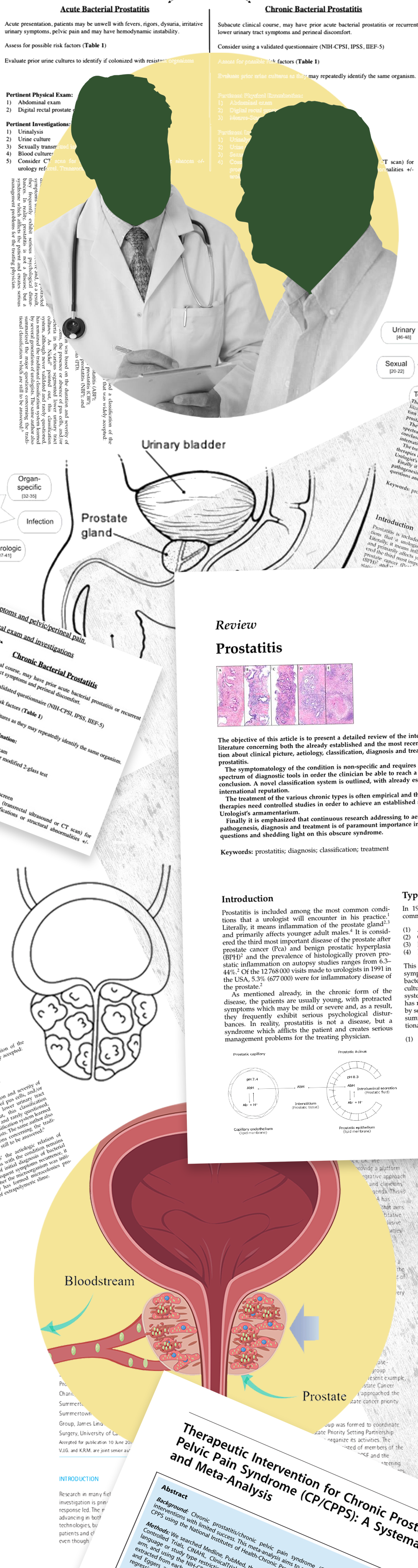
Prostatitis refers to inflammation or infection of the prostate gland, which lies just below the bladder and surrounds the urethra. It can cause painful or difficult urination, pelvic or genital pain, and other discomforts. There are four main types:
Acute bacterial prostatitis
Chronic bacterial prostatitis
Chronic prostatitis / chronic pelvic pain syndrome (CPPS)
Asymptomatic inflammatory prostatitis
Consult a doctor if you experience:
Slow or painful urination, dribbling, or difficulty starting or stopping your urine stream
Frequent urination, particularly at night, urgent needs to urinate
Pelvic, groin, or lower back pain
Cloudy or bloody urine, pain during ejaculation, or fever and chills (in acute cases)
You may need to provide:
A urine sample for infection checks
A blood test for inflammatory markers
A digital rectal exam (DRE) for prostate examination
Post-prostatic fluid urine test in certain cases
If symptoms persist without infection signs, further imaging or urodynamic tests may be advised
Acute bacterial prostatitis: Often treated promptly with IV or oral antibiotics for 2–4 weeks
Chronic bacterial prostatitis: Requires antibiotics (e.g., fluoroquinolones) for 4–12 weeks; resistant cases may need long-term suppression or surgical options such as TURP as a last resort
Chronic Pelvic Pain Syndrome (CPPS): May benefit from alpha-blockers, NSAIDs, pain control, and supportive therapy
Acute cases respond within days to a few weeks
Chronic cases may take several weeks to months for improvement
Medications and supportive therapies typically ease symptoms gradually
Acute prostatitis: May lead to blood infections, abscesses, or urinary retention if untreated
Chronic prostatitis / CPPS: Can result in depression, sexual dysfunction, infertility, and recurring pain
Antibiotics resolve most bacterial cases; chronic conditions may require longer therapy or multidisciplinary approaches
CPPS management may improve symptoms through medication and lifestyle support
Stay hydrated, minimize caffeine/alcohol/spicy foods
Practice pelvic relaxation or pain relief measures (e.g., warm baths)
Attend follow-ups and repeat tests as advised
Urologist: Diagnoses and leads treatment
Nursing staff: Guides home care and medication adherence
Psychologist/Pain Specialist: For chronic symptoms and associated stress
KKI stays updated on evolving treatments like precision antimicrobial therapies, pelvic pain rehabilitation, and advanced diagnostics.